We all want the best, most accurate information we can get regarding our health. And when the doctors and therapists are not getting the results everybody wants, they will typically order imaging studies to gather more information and an “accurate” look at what is going on.
Many in the general public consider the MRI as the gold standard or best possible diagnostic available. What we must realize, however is that an MRI (magnetic resonance imaging) is an image or picture. And as such, its interpretation relies on the individual reading the image. This is generally a radiologist but may also be another medical doctor that is treating you.
The technology behind an MRI is quite amazing and is not in question. What is of concern is the accuracy of the conclusions reached and therefore the ensuing treatment plan, costs and expected outcome(s)that follow.
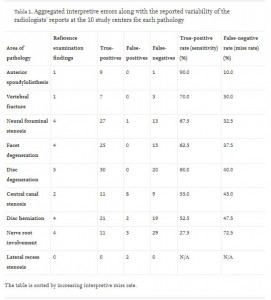
A 2017 study in The Spine Journal, wanted to look at just how accurate and consistent MRI findings would be across 10 different MRI centers. A 63-year-old women with a history of lower back pain and nerve pain down her leg received 10 MRI’s at 10 different locations over the course of 3 weeks.
What they found were very large differences in what was reported as the findings on the MRI in both false positives and false negatives (see chart from study below). Using disc herniation for example, 47.5% had a false negative or miss rate. Meaning the herniated disc was there but missed by the radiologist.
For those of us that work with a population determined to overcome their pain, the MRI is a double-edged sword. Because, as you may know from some of my past posts, the findings on an MRI do not have a one-to-one correlation with pain. There are people who have MRI’s that looked like they have been hit by a bus and have no pain. And there are people who have no clear findings on an MRI and may have significant pain. The bio-psycho-social factors that contribute to the pain experience are numerous.
What Can We Do?
Most importantly be informed and question everything. Even if you are sure the MRI findings are accurate, they don’t equate to surgery. In the absence of any medical emergency (significant muscle weakness, bowel or bladder problems), conservative treatment has shown to be as good as surgery and in several studies having even better outcomes.
At Function First, we are not doctors or physical therapists. We are exercise and movement professionals who understand the pain experience and how important it is to provide exercises that remove mechanical stress from the body and restore movement confidence through a very systematic process of program design and coaching.
When you seek help from a practitioner, you always want to be the head coach. And appreciate that passive treatments (hands on therapy, modalities) and medications may be necessary to progress you to the next step. But a comprehensive exercise program is ultimately what translates to the real-life functions you seek to participate in and enjoy.
Tags: biopyschosocial, lower back pain, MRI
are neurosurgeon and neurologist the same
Hi. No they are not, although both are highly trained in the nervous system. Only the neurosurgeon will operate, although I guess it is possible one could be both. Surgery can sometimes be an orthopedic issue with neurological consequences.